Get Answers
What Is an Endoscopic Ultrasound (EUS)?
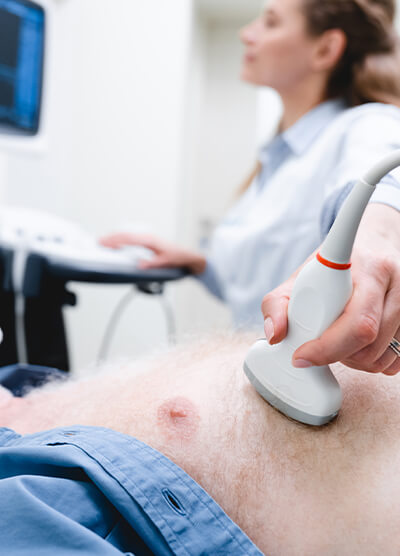
This procedure utilizes an endoscope and sound waves to obtain high-quality ultrasound images of the upper digestive tract in order to screen for diseases like hidden gallstones, and to evaluate possible tumors.
An endoscopic ultrasound (EUS) is a very sensitive test. It is used to obtain information for a diagnosis when other tests are inconclusive. It is also used to help decide on the best course of treatment – such as when or if to start chemotherapy or undergo surgery in the event of precancerous or cancerous lesions.
How Do I Prepare for My Procedure?
Your doctor will want to know about your health status, especially if you have allergies or other health problems such as heart disease, lung disease, or diabetes. If there is a possibility of fine needle aspiration, which is a type of tissue sampling done during an EUS, your doctor will want to check your blood for proper clotting. It is important to inform your doctor of any family history of bleeding problems or if you are taking medications that interfere with blood clotting (such as Coumadin, Xarelto) or platelet function (such as aspirin, Plavix, Advil, Aleve, or other NSAIDs). The wisest approach is to inform your doctor of any and all prescription and nonprescription medications you take.
EUS is performed with sedation administered by an anesthesia professional, so you will not be able to return to work or drive until the day after your procedure. This also means you will need someone to take you home, since EUS is an outpatient procedure. You will need to have an empty stomach on the day of the EUS, which means no food intake for 6 or more hours and no liquids for at least 2 hours. In case of a rectal EUS, you will probably need to take enemas or laxatives. In either case, full instructions will be given to you.
How Is the Procedure Performed?
For upper GI procedures, after IV sedation has been started, your physician will guide the endoscope with a tiny video camera into your mouth and esophagus. A similar instrument is used via the rectum for lower GI procedures.
Your physician will observe the inside of your intestinal tract on a monitor during the procedure and the ultrasound image on special equipment, and any findings will be recorded. The entire procedure generally takes 30 to 60 minutes, depending on its complexity and whether fine needle aspiration is performed. Sometimes, medications are injected – for example, as part of pancreatic cancer treatment.
What Can I Expect After My Procedure?
What Are the Risks Involved With the Procedure?
Like other endoscopy procedures, EUS is safe and well-tolerated. No procedure is without risk, but complications with EUS are quite rare. The complication rate for an EUS without fine needle aspiration is about 1 in 2,000, which is similar to the complication rate involved with other endoscopy procedures. Sometimes, patients may develop reactions to the medications used during EUS such as hives, rash, or nausea. The main complication is a tear (perforation) in the intestinal wall that requires surgical repair. This is quite rare, however, and precautions are taken to avoid it. Infection or bleeding after an EUS are also very rare.
What Are My Alternatives to This Procedure?
For patients with suspected cancer, a biopsy is needed to confirm the diagnosis before any treatment can be started. CT scan or conventional ultrasound-guided biopsies are good methods for tumors close to the skin. However, an EUS is safer and more accurate for “deep” tumors, such as those found in the pancreas or bile ducts.
During an EUS, your doctor can obtain the needed biopsies by extracting a small number of cells from across the digestive tract (esophagus, stomach, intestines and rectum), which avoids damaging overlying vital organs and blood vessels.
Surgery is an alternative to EUS, but it is much more invasive and requires general anesthesia, which carries its own set of risks.
Want more information about an upcoming endoscopic ultrasound (EUS)? Call the location nearest you.